Islet Research
We love islets!

Future therapy for diabetes: Save the beta-cell!
The Islet Biology Laboratory within the Centre for Biomolecular Interactions Bremen, University of Bremen is a purpose built islet research center, especially for diabetes research and includes research facilities for fundamental molecular and cellular biology and metabolism and for translational, human disease relevant research.
Concurrent with obesity, the global incidence of diabetes is increasing at an alarming rate, currently more than 420 Million people have diabetes. Our Lab seeks for a better mechanistic understanding of how the disease develops and for successful strategies to stop this epidemic.
Pancreatic β-cell death is the fundamental cause of type 1 diabetes (T1D) and a contributing factor to the reduced β-cell mass in type 2 diabetes (T2D). In both cases the mechanisms of beta-cell death are complex and as yet not fully defined. Modulation of apoptosis and identification of its stimuli is our approach towards the treatment of this metabolic disorder. Novel agents that can selectively block beta-cell apoptosis are urgently needed, since current therapies are directed towards alleviating only the symptoms and not the cause of the disease.
We work interdisciplinary and with multiple cellular in vitro and in vivo experimental models up to human autopsy and biopsy tissue. The identification of environmental factors, which lead to the disease is the 1st step towards its intervention. We look at viral and inflammatory pathways and the beta-cells’ response to stress, hyperactivation and hypernutrition.
The beta-cell has a very limited capacity to compensate for such environmental stress factors. With the identification of disturbances in the Hippo developmental pathway, we hope to induce beta-cell restoration and regeneration and thus, reversal of the disease in future.

We are a member of the Initiative Transparent Animal Research
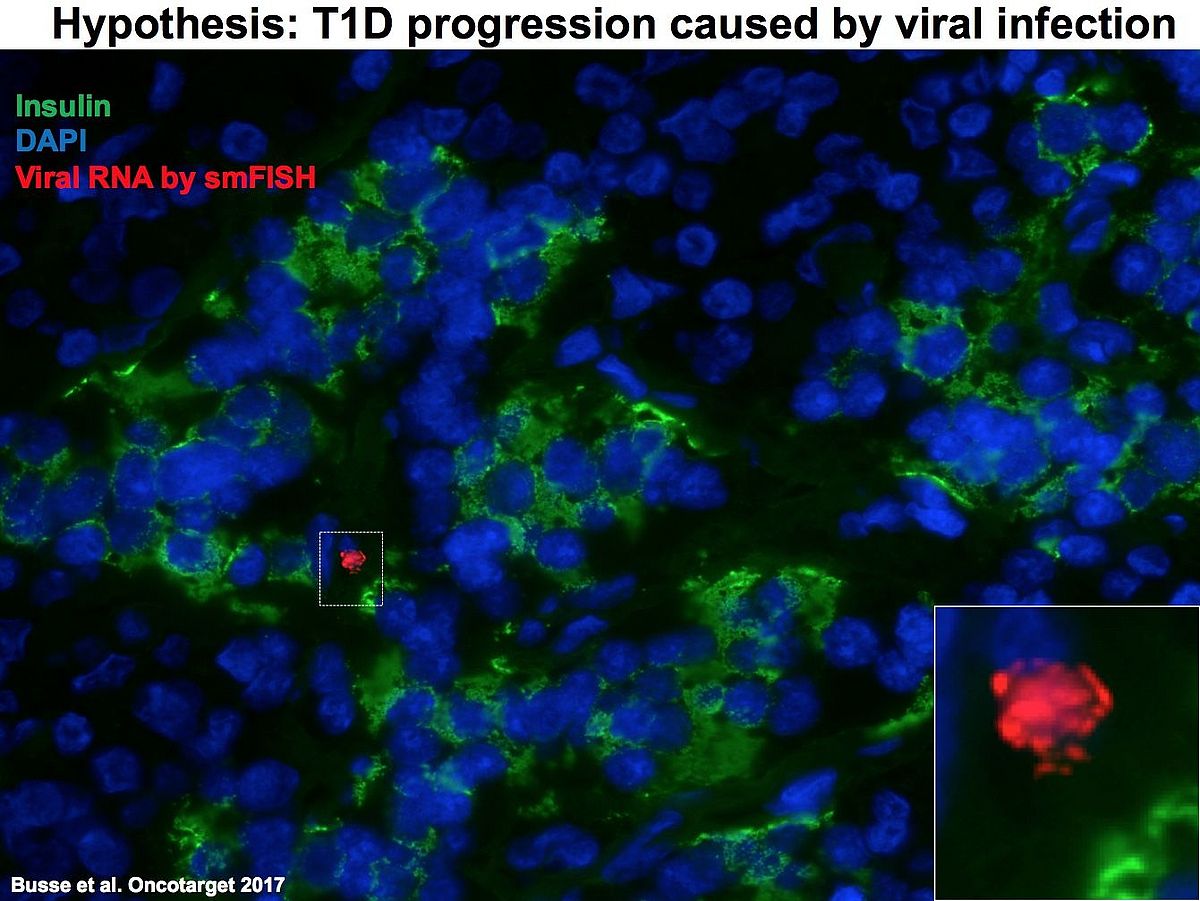
Enteroviruses, specifically of the Coxsackie B virus family, may directly trigger islet autoimmunity and type 1 diabetes, but their detection in the pancreas has been difficult.
Here we designed a panel of fluorescently labeled oligonucleotide probes, which specifically bind to the enteroviral genome of the picornaviridae family. They allow detection of very low copies of the virus genome in tissue samples from T1D patients. With these probes enteroviral RNA was detected with high sensitivity and specificity in infected cells and tissues.
Further recent in depth analysis of mechanisms of EV-mediated beta-cell destruction identified strong association of islet cell infection and beta-cell death and dysfunction. Our current work has identified specific virus localization in the pancreas in autoimmunity and in Type 1 Diabetes.
The HIPPO pathway: physiological regulator of beta-cell survival and function
For a successful therapy both, beta cell death as well as their loss of function needs to be targeted. Beta cell loss is causative for all types of diabetes and thus, the elucidation of the molecular processes associated with beta cell apoptosis and maintenance of beta cell mass is critical to develop new therapeutic strategies to prevent and/or delay these pathological events, since current treatment strategies do not -yet- include the preservation of the endogenous beta cell mass. Inhibiting pro-apoptotic or potentiating anti-apoptotic signaling can serve as potential strategy for restoring beta cell survival in diabetes.
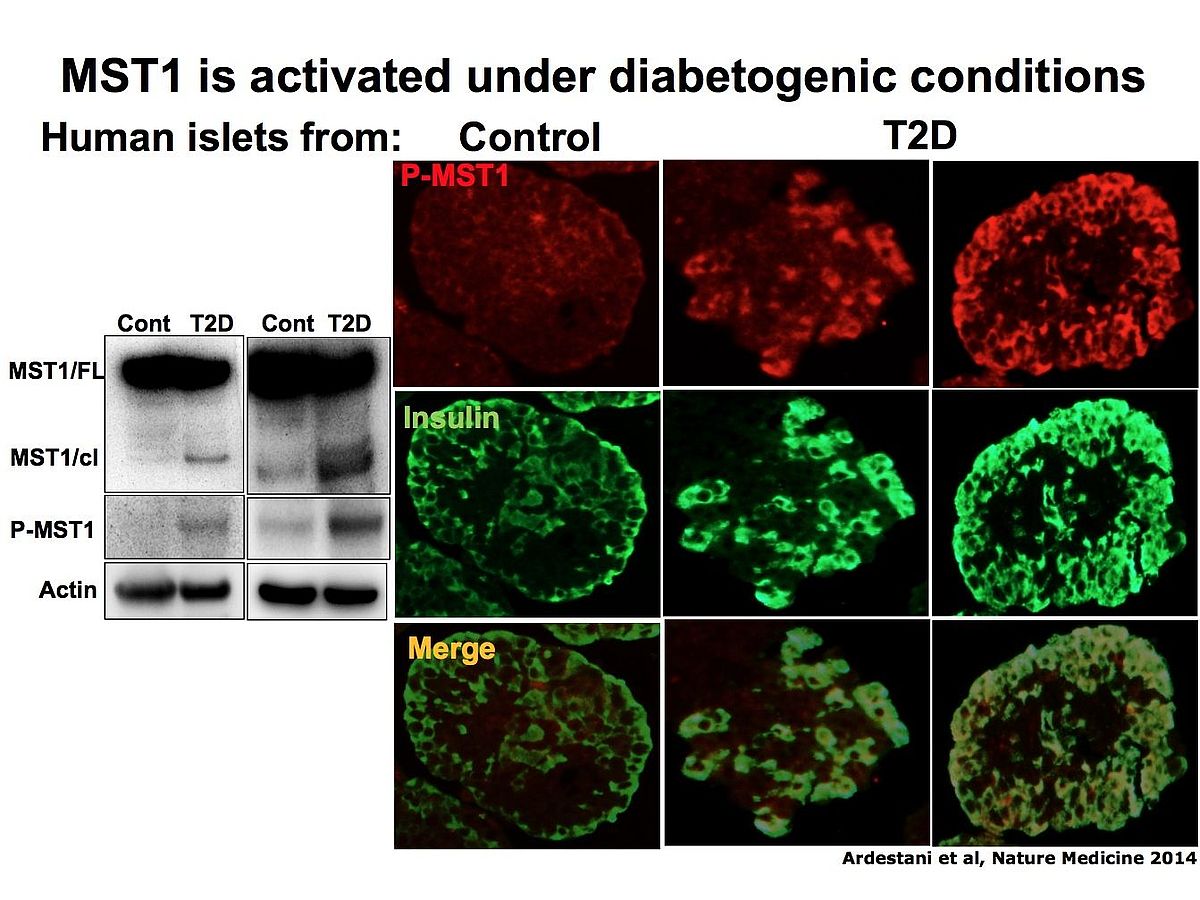
We identified the serine/threonine kinase Mammalian Sterile 20-like kinase 1 (MST1) as a critical regulator of apoptotic beta cell death and dysfunction. MST1 activates several apoptotic signaling pathways, leading to a vicious cycle of cell death.
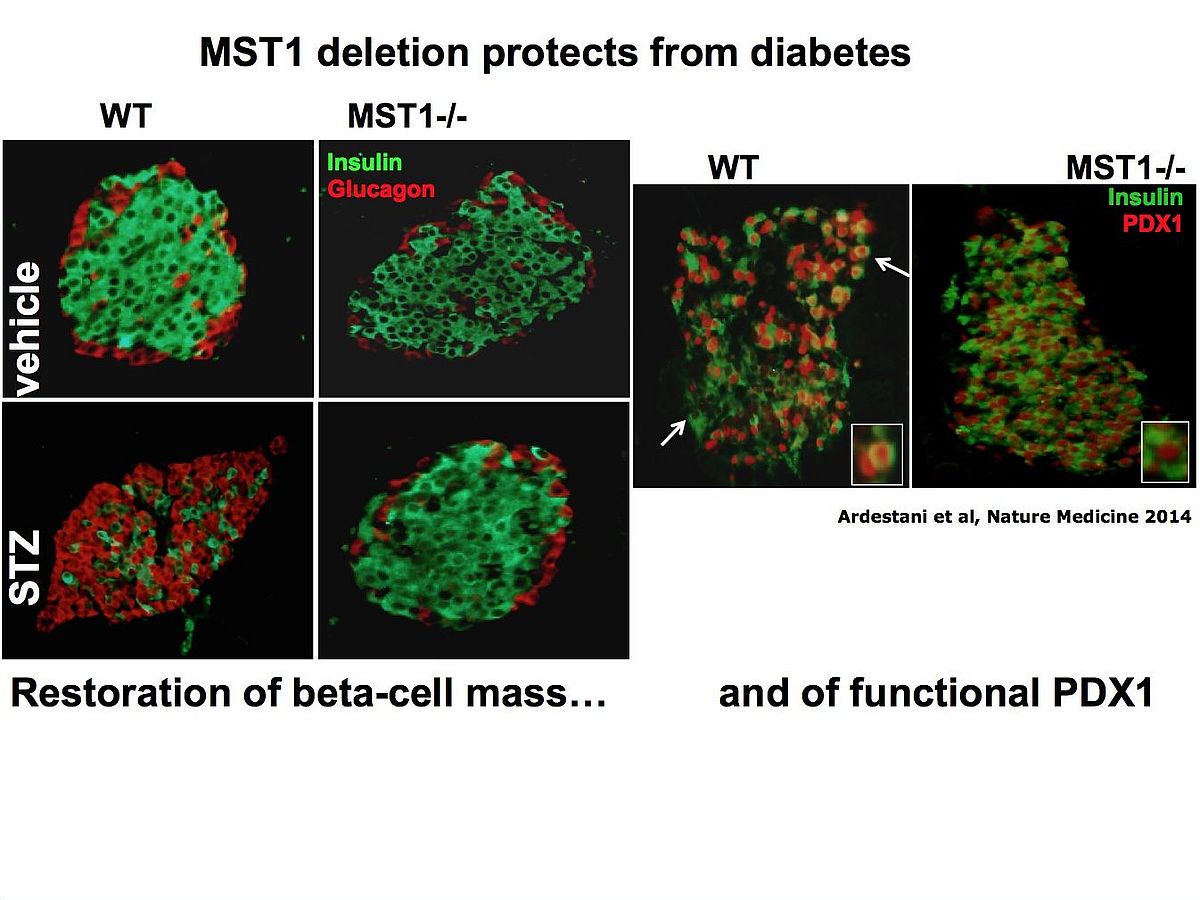
We found that MST1 is strongly activated in a diabetic beta cell and induces not only its death but also impairs insulin secretion through promoting proteasomal degradation of key beta cell transcription factor PDX1 which is critical for insulin gene expression.
Pre-clinical studies in various diabetic animal models show that MST1 deficiency remarkably restores normoglycemia and beta cell function and prevents the development of diabetes. Importantly, MST1 deficiency can also restore survival in already fully diabetic beta cells.
LATS: another Kinase in the Hippo pathway which regulates beta-cell survival

Large-tumor suppressor 2 (LATS2), a kinase and core component of the Hippo signaling pathway, is
activated under diabetic conditions and induces β-cell apoptosis and impaired function.
LATS2 deficiency in β-cells improves β-cell viability, insulin secretion and β-cell mass and ameliorates
diabetes development.
LATS2 activates mechanistic target of rapamycin complex 1(mTORC1), a physiological suppressor of autophagy.
Inhibition of mTORC1 counteracts the pro-apoptotic action of activated LATS2.
LATS2 is an autophagy substrate: a stress-sensitive multicomponent cellular LOOP: LATS2 regulates β-cell apoptosis triggered by impaired autophagy.
LATS2 is a potential therapeutic target to improve pancreatic β-cell survival and function in diabetes. (see full paper)
What happens downstream of HIPPO kinases MST & LATS?
Can we induce beta-cell regeneration by re-expressing the Hippo terminator YAP?
The essential points toward the investigations of Hippo functions in the beta-cell:
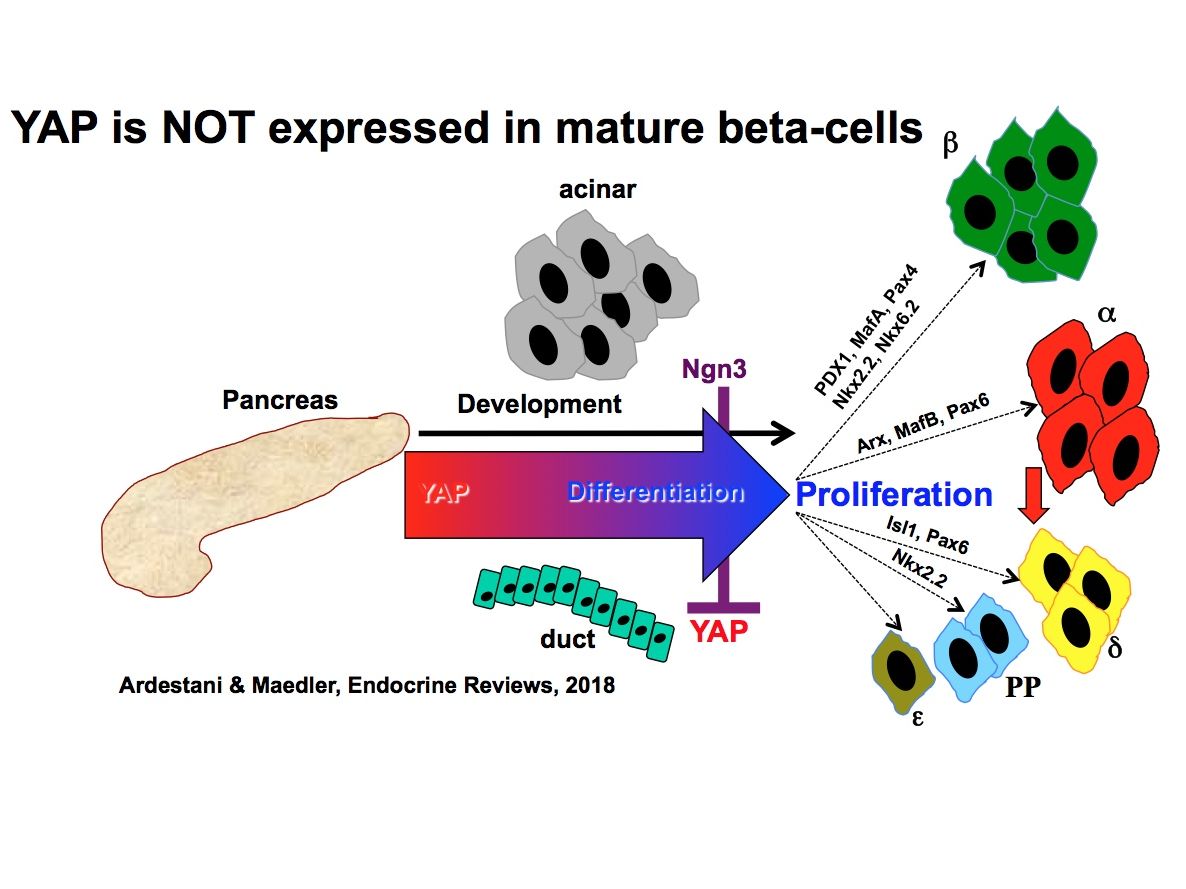
• The Hippo pathway regulates pancreas development including pancreatic progenitor cell proliferation, cell specification and differentiation as well as growth and cellular plasticity of the pancreas.
• Hippo pathway components control various aspects of β-cell homeostasis including beta-cell function, survival and proliferation.
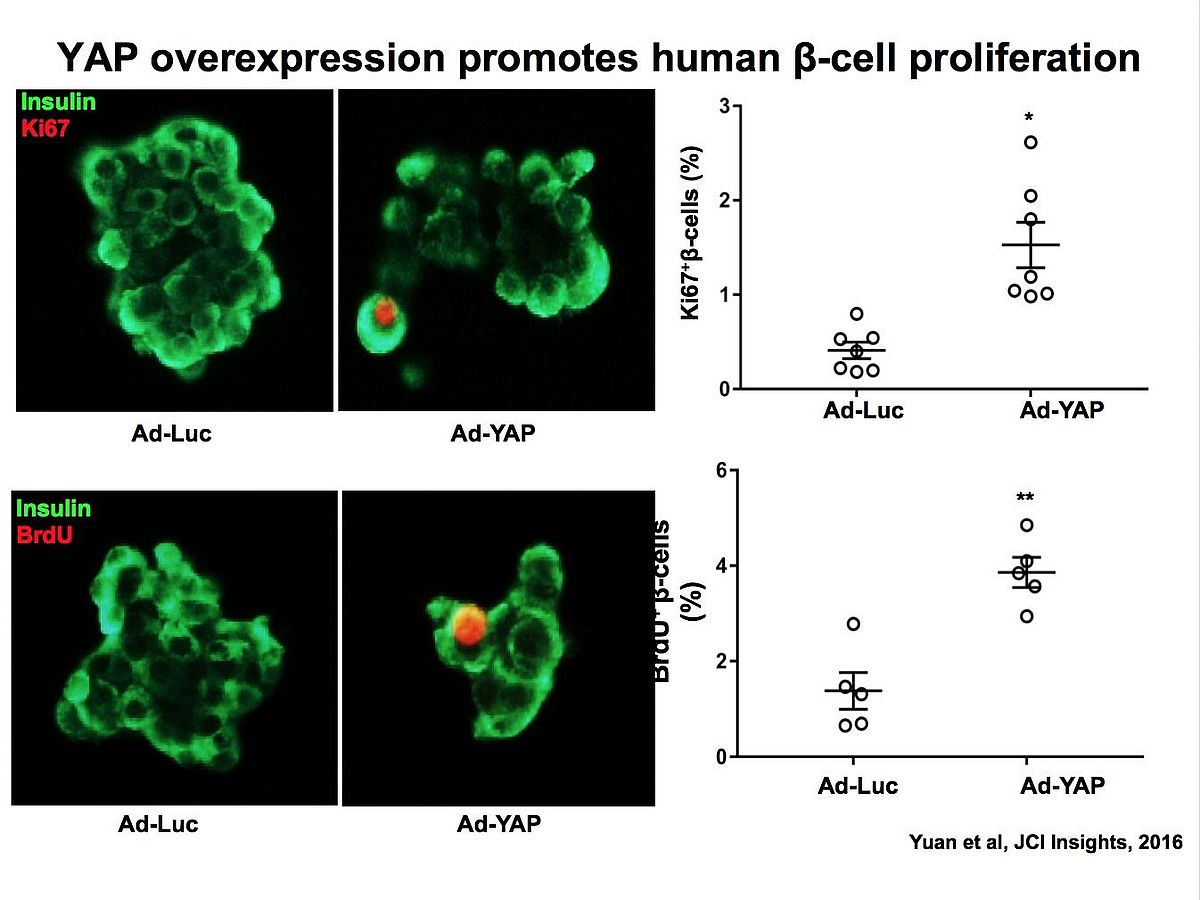
• The Hippo terminal effector YAP is not expressed in mature endocrine islet cells and its reconstitution promotes β-cell proliferation and survival.
• Targeting Hippo pathway could be an essential therapeutic approach for β-cell regenerative therapy.
Hippo Signaling: Key Emerging Pathway in Cellular and Whole-Body Metabolism. Trends EndocrinolMetab. 2018
PHLPP: The upstream regulator of HIPPO
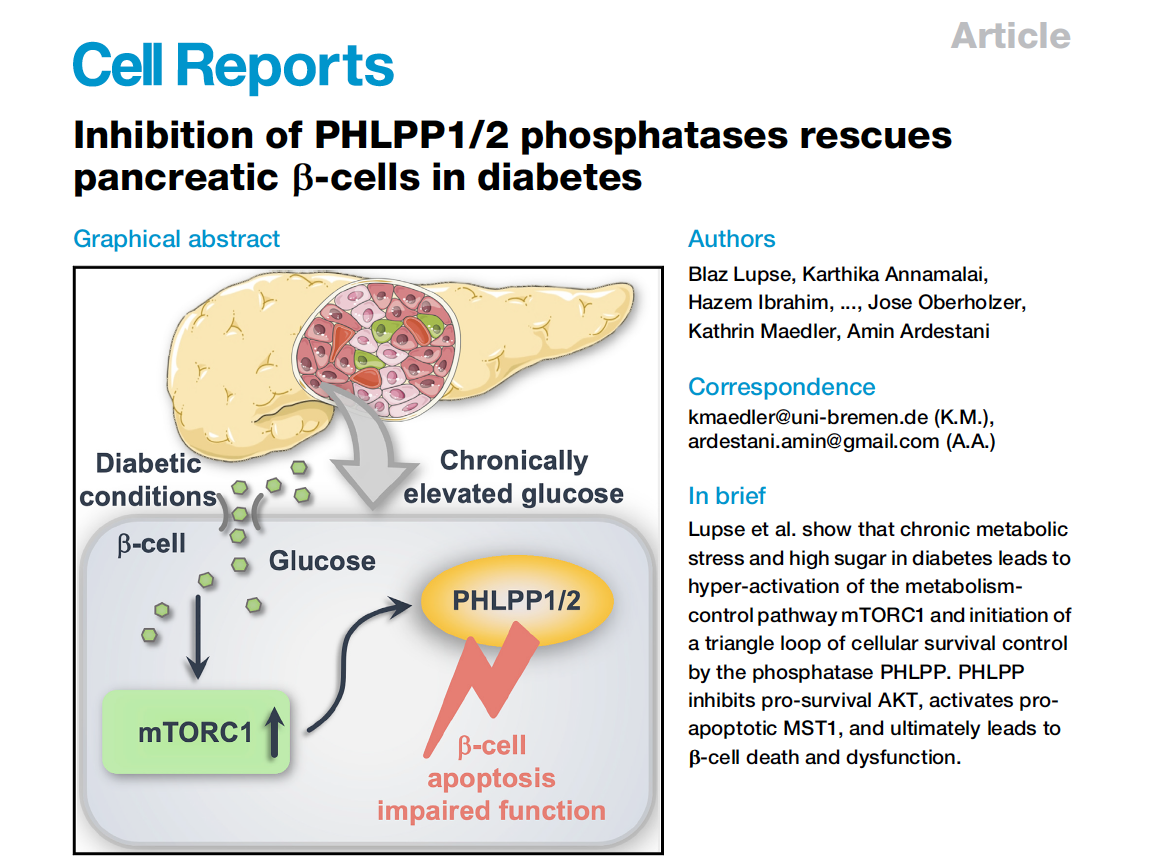
PHLPPs are highly elevated in metabolically stressed beta-cells in diabetes
Metabolic-stress-induced mTORC1 hyper-activation leads to PHLPP upregulation
PHLPPs regulate beta-cell survival-dependent kinases AKT and MST1
PHLPP inhibition restores glycemia, beta-cell survival and function
Diabetes: diseases of chronically elevated low-grade inflammation
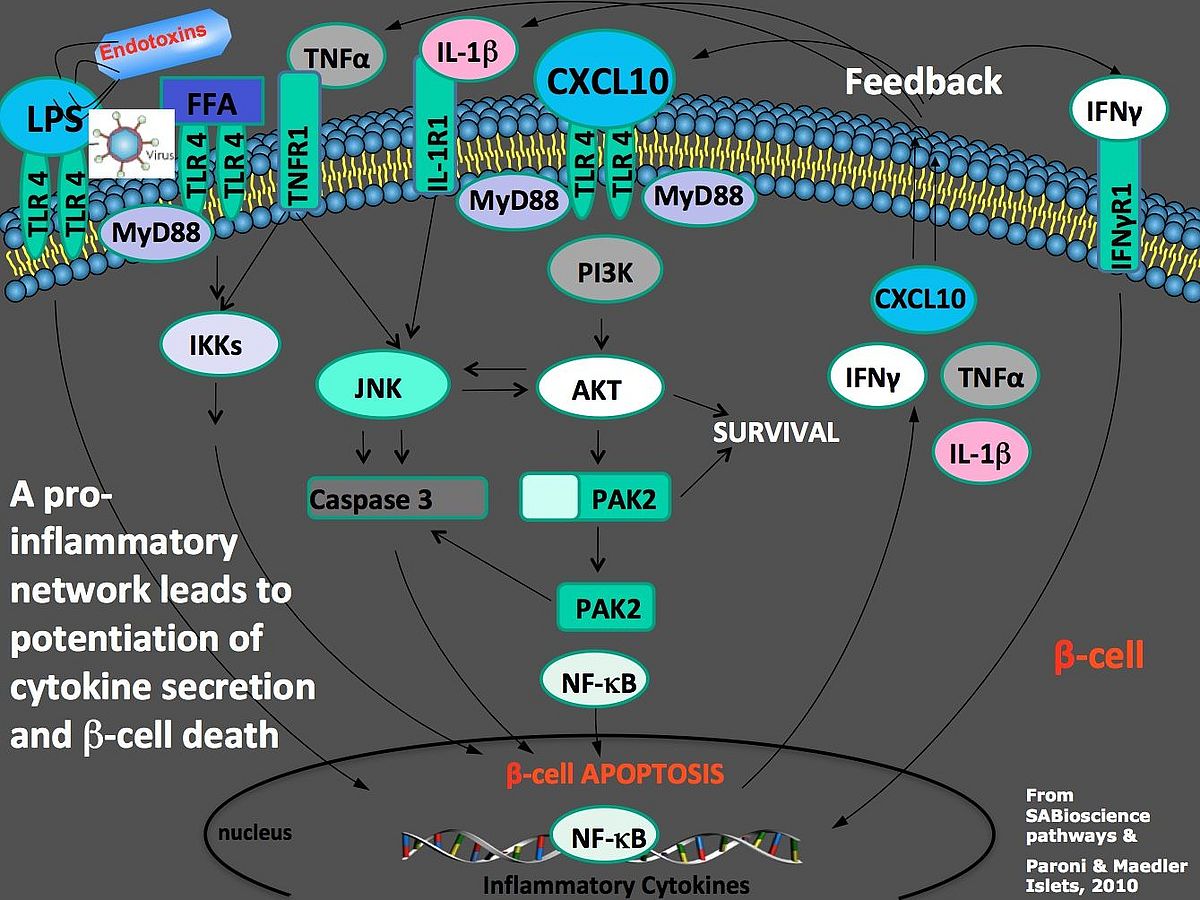
Secreted pro-inflammatory cytokines and chemokines into the proximity of the β-cell induce their destruction and impair insulin secretion. Several studies show that through several stimuli, intra-islet inflammation is causative for β-cell failure in both Type 1 and Type 2 Diabetes. A pro-inflammatory network then leads to potentiation of cytokine secretion and b-cell death
Only a combination of blocking immune-mediated beta-cell destruction together with restoration of beta-cell survival may therefore be successful strategy for future diabetes therapy.
Wei He et al., TLR4 triggered complex inflammation in human pancreatic islets. BBA Molecular Basis of Disease 2018





